
Angel M. Davey, PhD

Angel M. Davey, PhD
Health Science Program Manager
Tick-Borne Disease Research Program
Congressionally Directed Medical Research Programs
Fort Detrick, MD
Tick-Borne Disease Research Program


Angel M. Davey, PhD
Health Science Program Manager
Tick-Borne Disease Research Program
Congressionally Directed Medical Research Programs
Fort Detrick, MD
Tick-Borne Disease Research Program


The Cureus Journal (Aydin, Y., et al.) 07.07.2023, published “Severe Anaplasmosis With Multiorgan Involvement in a Rheumatoid Arthritis Patient.” This case report is of a 66-year-old woman from Connecticut with severe anaplasmosis. Anaplasmosis is an emerging tick-borne disease caused by the bacterium Anaplasma phagocytophilum, primarily transmitted through the bite of a black-legged tick, including Ixodes scapularis and Ixodes pacificus. Anaplasmosis is more common in certain US regions, including the upper Midwest, Northeast, and mid-Atlantic states, and most reported in Connecticut.

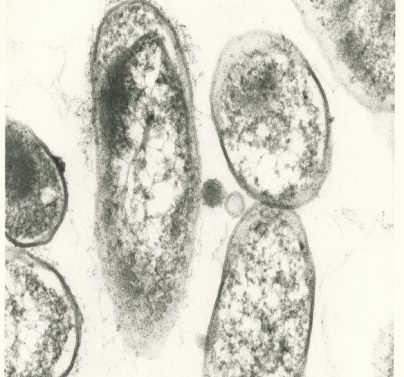
Open Forum Infectious Diseases (Ordaya E., et al.) 5.29.23 published “‘Let the Cat Out of the Heart’: Clinical Characteristics of Patients Presenting With Blood Culture-Negative Endocarditis Due to Bartonella Species.” The study was performed in an effort to define the clinical features of patients with Blood Culture-Negative Endocarditis (BCNE) due to Bartonella spp at Mayo Clinic in Rochester, Minnesota.

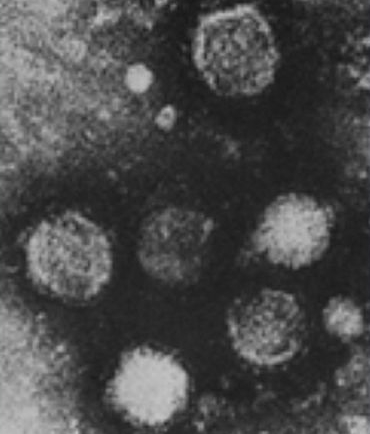
The Clinical Infectious Diseases Journal (Mendoza M. A., et al.) 08.04.2023, published “Powassan virus encephalitis: a tertiary center experience.” In this study, the researchers collected and analyzed clinical and epidemiological data from patients who had been diagnosed with neuroinvasive POWV infection from a study conducted at the Mayo Clinic from 2013 to 2022.
Powassan virus (POWV) is a type of flavivirus that is transmitted by Ixodes spp ticks. This virus has been recognized as an emerging pathogen that can cause neuroinvasive diseases, which affect the nervous system, and can lead to serious outcomes. The study identified sixteen patients who had been infected with neuroinvasive POWV. Within 90 days of diagnosis, three cases (18.8%) resulted in the patients’ deaths. Among the survivors, eight patients (72.7%) experienced residual neurological deficits, indicating lasting effects on their nervous systems.


The Pathogens Journal (Bush J. C., et al.) 07.18.2023, published “Viability and Desiccation Resistance of Bartonella henselae in Biological and Non-Biological Fluids: Evidence for Pathogen Environmental Stability.” The aim of this study is to understand Bartonella henselae‘s ability to survive in various fluids outside its host, which could potentially lead to infections in both animals and humans through environmental exposure. The researchers tested feline whole blood, serum, and urine, as well as bovine milk and physiologic saline (to simulate coastal marine conditions).


There are two new reports published by the CDC’s journal Morbidity and Mortality Weekly Report (MMWR) on alpha-gal syndrome (AGS), also known as the red meat allergy. AGS is an emerging tick bite associated allergic condition to most mammalian meat. These reports highlight that “AGS is of increasing concern for public health, but many healthcare providers (HCPs) are unaware of the condition and how to diagnose or manage it.”
The Morbidity and Mortality Weekly Report (Thompson, J. M., et al.) 07.28.2023, published the first report “Geographic Distribution of Suspected Alpha-gal Syndrome Cases — United States, January 2017-December 2022.” This report aims to make public health agencies and healthcare providers aware of AGS case hotspots in the United States in order to recognize the impact AGS is having in the country. Most cases were reported in the southern, midwestern, and mid-Atlantic United States.
The Morbidity and Mortality Weekly Report (Carpenter, A., et al.) 07.28.2023, published the second report “Health Care Provider Knowledge Regarding Alpha-gal Syndrome — United States, March–May 2022.” This report is the first national survey to assess healthcare provider’s knowledge of AGS. Approximately 42% of the United State’s Healthcare providers had never heard of AGS, with only 29% of providers who knew of the condition knowledgeable to diagnosis it. The report highlights the need for further awareness and education of AGS to help improve patient care in the United States.
The CDC, in collaboration with Medscape, is providing a free CME/CE training so learners are better able to self-assess gaps in their knowledge regarding the diagnosis and management of patients with AGS. Providers can access the training below.

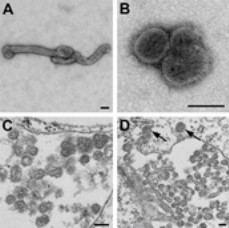
The Microorganisms Journal (Lange R. E., et al.) 06.12.2023, published “Diversification of Bourbon Virus in New York State.”
This study aims to clarify the genetic characteristics of Bourbon virus (BRBV) strains from New York State. The study identified two different strains of BRBV in New York State and suggests that these strains could “contribute to increased spread of BRBV in the northeastern US.”
The Bourbon virus is a tickborne virus that was first identified in Bourbon County Kansas, and is known to be detected in the lower midwestern US. But since 2020, the Bourbon virus has been reported in eastern states including North Carolina, Virginia, New Jersey, and New York State.

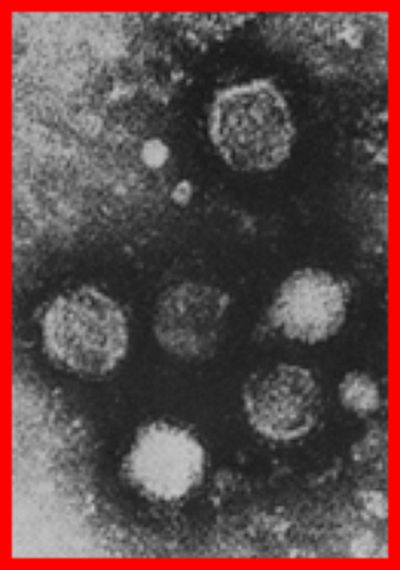
The American Society for Microbiology Journal (Telford S. R. & Piantadosi A. L.) 06.20.2023, published “Powassan virus persistence after acute infection.”
This study aims to better understand the neurological lasting effects after contracting Powassan encephalitis. This is done by observing the effects of Powassan virus (POWV) in mice. Powassan encephalitis is a severe tickborne virus with a high mortality rate and lasting symptoms in many individuals after recovery.
POWV in humans is “notable for the severity of both the acute disease and the long-term sequelae.” Acute infection symptoms include fever and fatigue, but 95% of cases are neuroinvasive, meaning it causes infection in the brain (encephalitis).


An article regarding recent study on effectiveness of permethrin-treated uniforms against ticks was conducted at Department of Defense (DOD) Military Tick Identification/Infection Confirmation Kit Program (MilTICK program) was published by […]

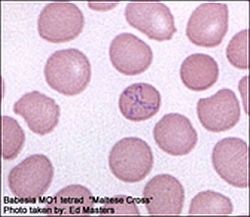
The Emerging Infectious Diseases Journal (Locke, S, et al.) 06.2023, published “Neurologic Complications of Babesiosis, United States, 2011–2021.” This study aims to describe the “neurological complications of babesiosis in a group of hospitalized patients” from Connecticut. Babesiosis is a parasitic infection that is primarily transmitted through the bite of an infected ixodid tick.
LDA Doctor Referral System © Terms & Conditions and Guidelines
Save this Information for Your Records:
About LDA DOCTOR REFERRAL SYSTEM ©
Welcome to the Lyme Disease Association’s LDA Doctor Referral System ©. LDA made updates and enhancements to its prior system and has launched a new site to provide patients with information about doctors, other practitioners, testing labs, and pharmacies that are knowledgeable about chronic Lyme disease and often about many other tick-borne diseases (TBD). Many of the doctors listed are often referred to as Lyme Literate Physicians/Doctors (LLMD). Tens of thousands of patients have successfully used the prior LDA system to locate Lyme and TBD resources.
Terms & Conditions and Guidelines
Because there is a negative political climate surrounding Lyme disease, many LLMDs do not want their names posted outright on the internet. LDA has tried to balance the doctors’ wishes with patients’ need to find a doctor. This new system is a result of that compromise and therefore:
Because of the limited number of physicians treating chronic Lyme disease nationwide, some states, and in some instances, entire regions, may not have any treating physicians who follow flexible treating approaches such as those in the International Lyme & Associated Diseases Society (ILADS) Guidelines, Evidence Assessments and Guideline Recommendations in Lyme Disease: The Clinical Management of Known Tick Bites, Erythema Migrans Rashes and Persistent Disease. In the event that the LDA Doctor Referral System © contains no Lyme or TBD resource listings in a given area, the closest possible option(s) will populate based on the location entered and specaialty/ies selected. The LDA appreciates any changes in provider information that you may find and make us aware of so we can investigate.
Some providers may not specifically treat Lyme and TBD but see patients who have symptoms associated with Lyme and TBD to address those specific symptoms. Contact the provider to confirm.
It is your responsibility to contact the provider’s office to confirm the current address, directions, nature of services provided, and all other provider information before you make an appointment.
DISCLAIMER: The Lyme Disease Association, Inc. provides referrals to health care providers who treat Lyme disease, and often other TBD, as a courtesy to those seeking Lyme Literate Physicians (LLMD). However, some of the providers included do not specifically treat Lyme and TBD but see patients who have symptoms associated with Lyme and TBD to address those specific symptoms. We do not evaluate the professional competence or qualifications of health care providers on our referral list or the costs of services provided. Accordingly, the LDA neither warrants nor endorses the health care providers contained on this list nor the quality of care you will receive from those providers. We do not make recommendations, only referrals. LDA does not receive any monies from physicians to be included on this list nor does LDA provide any monies to physicians. Because of the limited number of physicians treating chronic Lyme disease nationwide, some states, and in some instances, entire regions, may not have any treating physicians who follow flexible treating approaches such as those in the International Lyme & Associated Diseases Society (ILADS) Guidelines: Evidence Assessments and Guideline Recommendations in Lyme Disease: The Clinical Management of Known Tick Bites, Erythema Migrans Rashes and Persistent Disease. In the event that the Doctor Referral System contains no Lyme or TBD resource listings in a given area, the closest possible option(s) will populate based on the zip code entered and category/ies selected. The LDA appreciates any changes in provider information that you may find and make us aware of.
LDA does not accept or reply to any comments on:
We cannot guarantee that the information provided will be timely and accurate or that physicians on the list are accepting new patients, or that they accept insurance. The selection of a physician should be made by you after careful consideration. There are two approaches in the treatment of Lyme disease. Our list contains physicians who generally follow more flexible treatment approaches than those advocated by the Infectious Diseases Society of America (IDSA). LDA is not responsible for incorrect information on the website. BEFORE DOCTOR VISIT: Please contact the physicians’ offices directly to confirm their current address, directions, and any other necessary information before scheduling an appointment. Do not rely only on the maps provided on this site. The maps on LDA’s Doctor Referral System are for informational purposes and provide an approximate locality of the listing based on the addresses we are provided with at the time of site updates. Practitioners often relocate and addresses can change. Notification of changes in listed information can be updated on our Dr. Referral Contact Form. Thank you, Lyme Disease Association, Inc. (LDA)
Subscriber information will not be shared outside of the Lyme Disease Association, Inc. nor used for donor solicitation.
The Lyme Disease Association, Inc. reserves the right to unsubscribe anyone from this service without cause.
